 Lieutenant Colonel Rebecca Hayes arrived at Riverside Regional Trauma Center with a résumé line that made people shift in their seats: three wars, zero panic.
Lieutenant Colonel Rebecca Hayes arrived at Riverside Regional Trauma Center with a résumé line that made people shift in their seats: three wars, zero panic.
At fifty-two, she moved with the careful efficiency of someone who had carried too many stretchers through sandstorms and smoke-filled compounds.
Her hands trembled slightly when she signed in, not from fear, but from an old nerve injury she never bothered to explain.
Riverside was famous for its rankings, its donors, and its residents who wore prestige like cologne.
On the first day, a young surgeon named Doctor Brandon Caldwell looked her over and smiled like he had already measured her limits.
“So you’re the military nurse,” he said, loud enough for half the hallway to hear, “did they send you here to teach us how to bark orders?”
Rebecca didn’t argue, because arguing wasted oxygen and time.
She stocked crash carts, checked seals, studied the hospital’s trauma protocols twice, and learned the rhythms of the staff the way she once memorized terrain maps.
Brandon watched her quiet discipline and mistook it for weakness.
By Day Two, the jokes turned into little tests.
Brandon “forgot” to introduce her during rounds, corrected her loudly in front of interns, and called her “ma’am” with the same tone a student uses for a substitute teacher.
Rebecca kept her voice calm, asking thoughtful questions that forced people to pause and think, then stepping back before egos could ignite.
On Day Four, she overheard Brandon in the break room with two residents.
He slapped a bill onto the table and said he’d pay five hundred dollars if Rebecca quit or made “one fatal mistake” before the week ended.
The room laughed, and that laughter followed Rebecca down the corridor like an echo meant to sting.
Doctor Margaret Ellis, a trauma attending with weary eyes and undeniable skill, noticed Rebecca’s stillness.
She didn’t defend her in public, but later she handed Rebecca a pager and said quietly, “Ignore the noise. Focus on the patient.”
Rebecca nodded, because respect in medicine often arrived in whispers instead of applause.
By Day Six, something in the air felt wrong from the start.
At 2:11 p.m., the radio at the charge desk crackled with the words every trauma center dreads: mass casualty incoming, military transport, multiple critical.
Rebecca’s spine straightened instantly, like a reflex she had never lost.
The bay doors rolled open, and the first gurney burst through at a run.
Navy SEALs came in with soot on their skin, blood staining their uniforms, and eyes that looked beyond the ceiling lights.
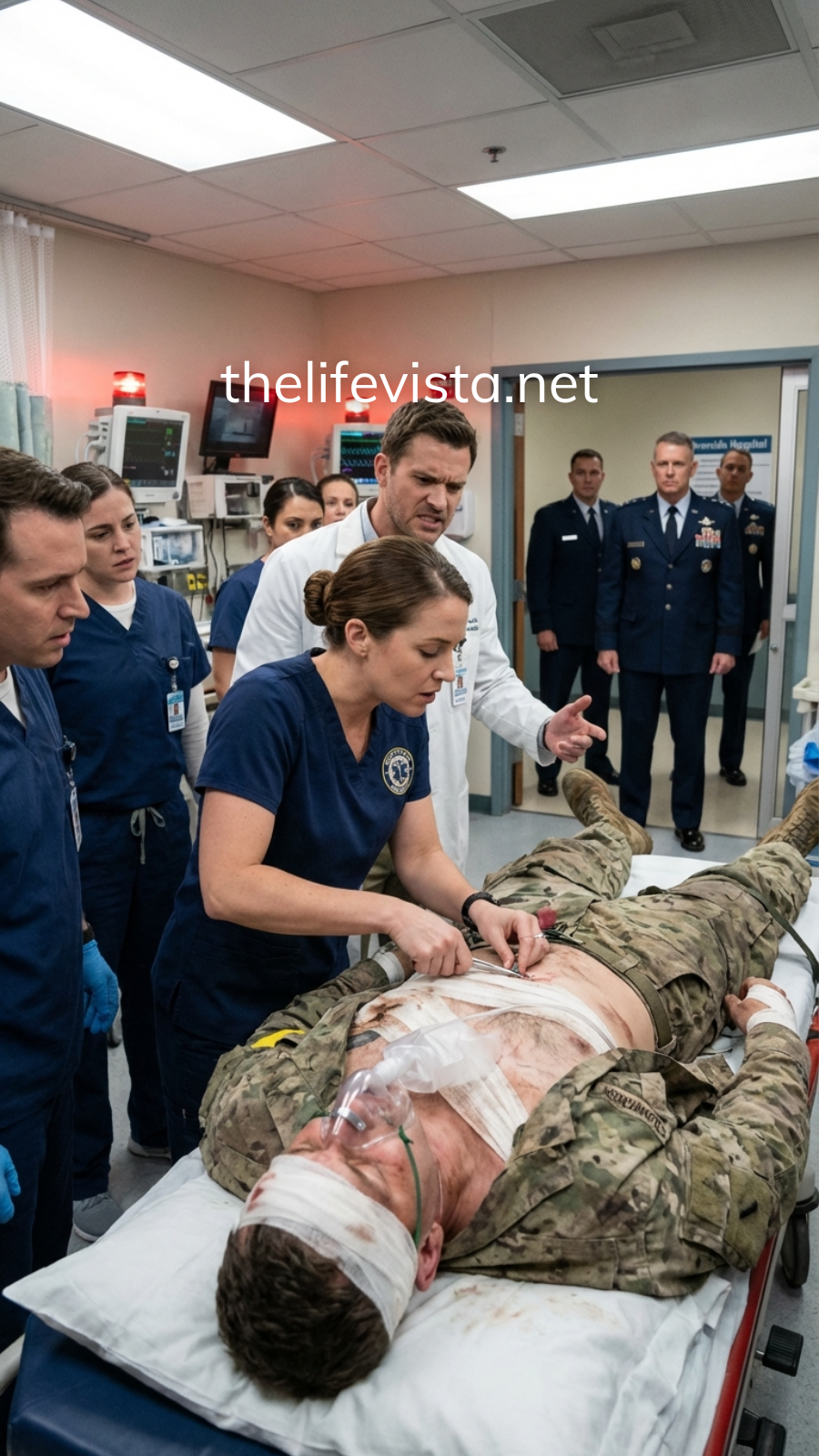
On the lead stretcher, Commander Daniel Brooks gasped for air that refused to fill his lungs, and Rebecca saw something the monitors weren’t saying out loud—was this the moment Riverside would discover what real battlefield experience meant?
The trauma bay exploded into motion, voices overlapping while gloves snapped and scissors cut through fabric.
Doctor Brandon Caldwell took the lead like it was his stage, calling orders with the confidence that made interns breathe easier.
Rebecca stayed near the head of the bed, watching the commander’s neck veins, the uneven lift of his chest, and the fear pressing through the sedation.
Commander Daniel Brooks’s left side barely moved.
His oxygen numbers dipped, climbed, then dipped again like a drowning swimmer breaking the surface for brief air.
Rebecca leaned closer and heard diminished breath sounds on one side, a detail that never required prestige to matter.
Brandon glanced at the ultrasound and declared it “messy but manageable.”
He blamed bruised ribs, blood loss, and stress, then ordered more fluids and faster transfusion.
Rebecca watched Brooks’s skin fade toward gray and felt a cold certainty settle in her chest.
She spoke once, calm and steady.
“Doctor Caldwell, this looks like a tension pneumothorax building,” she said. “His trachea is shifting and he’s crashing.”
Brandon’s head snapped toward her as if she’d insulted him in front of his own team.
“You’re a nurse,” Brandon said sharply. “Stay in your lane.”
Margaret Ellis hesitated, eyes flicking between the monitor and Rebecca’s face, caught between hierarchy and instinct.
Rebecca didn’t raise her voice, because the patient did not have time for hospital politics.
Brooks’s heart rate spiked, then faltered.
The commander clawed weakly at the oxygen mask, eyes wide with the raw terror of air starvation.
Rebecca felt the room tipping toward catastrophe and decided she would rather be fired than watch a man suffocate.
She reached for the emergency kit and moved with precise speed.
Brandon barked, “Do not touch him,” and a security officer near the door shifted as if already prepared to intervene.
Rebecca looked directly at Margaret Ellis and said, “If I’m wrong, I’ll walk out myself. If I’m right, he lives.”
Margaret’s silence lasted one heartbeat too long.
Rebecca acted, performing emergency decompression the only way battlefield medicine ever allowed—fast, decisive, and accountable.
A sharp rush of trapped air escaped, and Brooks’s chest began rising more evenly almost immediately.
The monitor stabilized enough for the room to breathe again.
A few interns stared at Rebecca as if gravity itself had just changed direction.
Brandon’s face flushed with anger, because she had been right where he had been certain.
“You just violated protocol,” Brandon snapped, stepping closer.
He turned to the charge nurse and said, “Call security. Remove her from my bay immediately.”
Margaret Ellis opened her mouth, then closed it, watching the commander’s color return while career calculations flickered behind her eyes.
Security moved in, hands out, as if Rebecca were a threat instead of the reason the patient still had a pulse.
Rebecca removed her gloves slowly to show she wasn’t resisting and kept her gaze on Brooks until the last moment.
As they escorted her toward the hallway, she heard Brandon boast loudly, “I told you she’d make a mistake.”
Then a monitor alarm shrieked from the trauma bay.
A nurse shouted vital numbers, another yelled “pressure dropping,” and the fragile calm shattered again.
Rebecca turned her head and saw Brooks’s chest failing once more, as if the danger had only paused.
She tried to step back inside, but security blocked her path.
Brandon shouted over the chaos, “Nobody moves until I say,” and his voice sounded more frightened than confident.
Rebecca watched from the corridor as hands hesitated, realizing pride might finish what trauma had started.
Then another sound echoed down the hall—boots, heavy, urgent, disciplined.
The doors opened and a tall four-star general stepped inside surrounded by aides, his expression carved from granite.
General Michael Donovan’s voice filled the corridor with a single sentence that froze everyone in place: “Where is Lieutenant Colonel Hayes, and why is my operator dying without her?”
General Michael Donovan didn’t raise his voice.
He looked from the security officers to Brandon Caldwell, then toward the trauma bay where alarms still wailed.
“Move,” he said quietly, and the word carried authority that outranked every title in the building.
Security stepped aside immediately.
Rebecca walked back into the bay without rushing, because rushing leads to mistakes and mistakes cost lives.
She assessed Brooks in a single sweep and saw what Brandon had missed again—ongoing pressure, incomplete stabilization, and the need for decisive intervention.
Margaret Ellis finally spoke.
“Rebecca, tell me what you need,” she said, sounding like a door finally opening.
Rebecca issued crisp instructions, guiding the team into a controlled sequence that replaced chaos with purpose.
Brooks’s vitals steadied the way a storm calms once the wind breaks.
The commander’s eyes met Rebecca’s briefly, and in that glance lived gratitude and the memory of how close he had come to death.
Rebecca reassured him not with words, but with competence.
Brandon tried to reclaim authority with louder commands.
General Donovan turned his head and fixed Brandon with a stare that stripped the room bare.
“Doctor Caldwell,” he said evenly, “step away from this patient and answer my questions as if your career depends on it.”
Brandon sputtered about protocol and chain of command.
Rebecca kept working, refusing to be dragged into debate while a human being struggled for oxygen.
Margaret Ellis backed Rebecca’s calls without hesitation, and that shift changed the entire room.
Outside the bay, Donovan demanded the incident report, the security call log, and supervisor notes.
An aide produced a screenshot from a resident group chat where Brandon’s five-hundred-dollar bet sat like a stain.
Donovan’s jaw tightened, and the air around him grew colder.
He walked back in and addressed the entire trauma bay.
“Riverside exists to save lives, not protect egos,” he said, then turned to Brandon.
“You ignored a life-threatening diagnosis, attempted to remove the clinician who corrected you, and treated a trauma bay like a casino table.”
Brandon tried to respond, but Donovan lifted a hand.
“Effective immediately, you are removed from patient care pending termination and investigation,” he said.
Then he turned to Rebecca and added, “Lieutenant Colonel Hayes, you are reinstated immediately. Brief me on what you observed.”
Rebecca explained the signs calmly, without drama.
She described the tracheal shift, the pressure buildup, and the urgency that seconds demanded.
Donovan nodded once and ordered hospital leadership to conduct an emergency review of training, escalation pathways, and staff culture.
The next morning, Riverside’s board arrived in suits, shocked that a four-star general had walked into their polished institution and reshaped it overnight.
Margaret Ellis spoke first, openly supporting Rebecca’s judgment and admitting her own hesitation had been dangerous.
Rebecca didn’t gloat, because medicine punishes arrogance faster than any courtroom.
Within a week, Donovan ordered a new operational standard across Riverside trauma care.
It was called the Phoenix Protocol, named after Rebecca’s battlefield call sign and the belief that hospitals must rise stronger from failure.
The protocol required team listening, mandatory cross-checks, and immediate escalation whenever any clinician identified a time-critical threat.
Rebecca became Director of Trauma Training and taught with quiet intensity.
Her simulations forced residents to practice humility, because humility keeps hands steady when fear arrives.
She never shamed anyone for inexperience, but she never excused carelessness either.
Six months later, Riverside’s mortality rate dropped dramatically, and staff stopped talking about pedigree as if it were oxygen.
Commander Daniel Brooks returned, walking slowly but upright, and shook Rebecca’s hand with steady gratitude.
“Out there we call this courage,” he told her. “In here you call it nursing, and that’s the difference.”
Rebecca’s hands still trembled some mornings.
But Riverside learned that trembling hands can still save lives when the mind is clear and the heart refuses to surrender.
If this story moved you, share it, comment your city, and thank a nurse today—because courage often lives in the quietest hands.




